Thyroid Disease
|
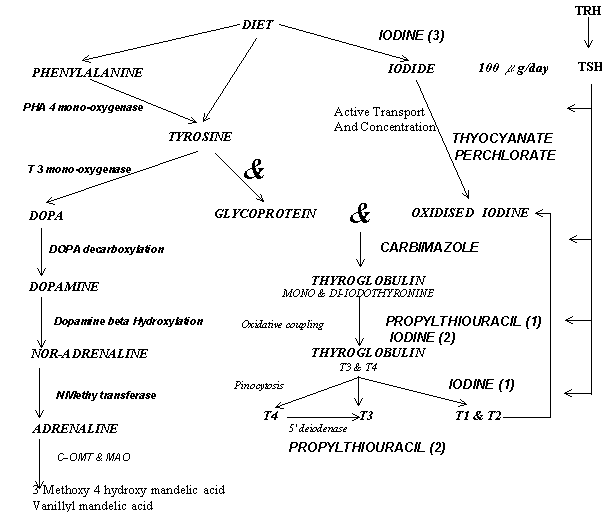
Physiology
Hormone |
Secretion
mg/day |
Level
mg/dl |
t 1/2 |
Onset |
Max effect |
Biological Effect |
T 4 |
80-100 |
4.5-10 |
7 dys |
3 dys |
10 dys |
T 4 Exerts its
effect by conversion to T 3 . This is dependent on nutritional, illness and
hormonal factors unrelated to thyroid status |
T 3 |
10 |
0.2 |
1 dy |
6 hrs |
2 dys |
rT 3 |
35 |
0 |
Biologically inactive |
T 3 becomes cellular protein bound to increase nuclear transcription of genes
leading to
- Increased Basal Metabolic Rate with Increased oxygen consumption,
- Increased respiratory rate and tidal volume
- Increased heat production.
- Increased blood supply with vasodilatation
- Increased blood volume
- Increased cardiac output and heart rate
- Increased protein catabolism leading to creatinuria, muscle weakness, osteoporosis and
increasing calcium and phosphate levels.
- Increased number of beta receptors and decreased number of cardiac cholinergic
receptors.
- Increased and uncoupled mentation.
| |
Thyrotoxicosis |
Myxoedema |
Causes |
Graves disease (TSI
- ?LATS), Paranodular graves, Multinodular goitre, Toxic nodule, Hypersecretion of TSH,
Excessive replacement - iatrogenic, intentional. |
Idiopathic,
Iatrogenic - Surgery, Radioactive iodine. Antithyroid R x. Iodine deficiency.
Hashimotos, DeQuivaines, Reidals thyroiditis
Drugs - Li, cholestryramine, SNP, Amiodarone, phenytoin, phenobarb |
Symptoms |
Fatigue, Weight
loss, Increased appetite, Heat intolerance, Palpitations,
sweating, anxiety, irritability, diarrhoea, Oligo/Amenorrhoea |
Weight gain,
Anorexia, Cold intolerance, fatigue, constipation, Menorrhagia, Dry skin, Hair loss |
Signs General |
Thin, anxious pt,
warm moist skin, palmar erythema, telangectasia, fine soft skin, hair, nails, clubbing
(acropachy), pretibial myxoedema |
Hypothermia, Puffy
face, Periorbital odema, large tongue, coarse dry skin, carotenaemia, hoarseness,
deafness, slow mentation, confusion,
coarse sparse hair, loss of outer third of eyebrows |
Cardiac |
SVT with atrial
fibrillation
Resting pulse > 90bpm
High output failure |
Sinus bradycardia,
small complexes,
CCF pleural and pericardial effusions |
Peripheral |
Fine static tremor,
Proximal myopathy |
Carpal tunnel syn.
Pendular reflexes |
Eye |
Lid retraction and
lag, Exopthalmos |
|
Other |
Osteoporosis |
Megaloblastic
anaemia |
Peri-operative management
Physiologically euthyroid state
Localisation of suspected hormone secreting tumours with documentation of hormonal
excess or deficiency
| |
T 4 |
TSH |
| Thyrotoxicosis |
� |
� |
| 1 o Hypothryroid |
� |
� |
| 2 o Hypothyroid |
� |
� |
| Pregnancy |
� |
N |
Thyrotoxicosis
Medical normalisation of hormonal status
- 2-6 weeks of stabilisation on a thionamide antithyroid agent.
They inhibit oxidation
and organification of iodide and the coupling of iodotyrosines. In high doses can inhibit
the peripheral conversion of T4 to T3 Carbimazole (Neomercazole) converted to Methimazole
(Trapazole) 5mg tablet 4-14hour half life. 20-60mg/day in 1-3 doses Propylthiouracil 50mg
tablet 1-2hour half life. 300-1200mg/day in 4 doses.
- Adrenergic antagonists to control the excessive autonomic stimulation.
Propanolol
(Inderal) 10mg tablet. 3-6 hour half life. 40-240mg/day in 4 doses Nadolol 16-24 hour half
life (Drug Of Choice - Hammilton, Forrest, Gunn - due to the long half life) Esmolol 50
microg/Kg ivi loading dose then 25-300 microg/Kg/min ivi until HR < 90bpm and
hypertension controlled
- Iodine acutely inhibits the release of T4 and transiently inhibits organification (Wolff
- Chaikoff effect).
Iodine was used to decrease the vasularity and the size of the
gland but it is not used by surgeons any more as it is associated with release of stored
hormone causing severe storm (Reed, Bradley).
Assessment and treatment of end organ disease
Cardiovascular
Resting heart rate is excellent guide to when to perform surgery.
ECG for arrhythmias, ischaemia and digoxin changes (Important in apathetic mxyoedema)
ECHO for Left Ventricular function as prolonged exposure to excess catecholamine
secretion will result in a cardiomyopathy
Respiratory
Careful history for symptoms of tracheal compression - Treat as for anterior
mediastinal mass. Careful examination for ease of intubation
- Chest X ray - Position and compression of trachea
- Flow volume loops lying and sitting
- CT scan of the Trachea
- ENT indirect laryngoscopy for documentation of recurrent laryngeal nerve involvement
Metabolic
- Haemoglobin - Anaemia contributes to cardiac decompensation.
- Platelets
- Coagulation status
- Urea and electrolytes
- Thyrotoxicosis is associated with diarrhoea and relative or absolute gluco and
mineralocorticoid deficiency
Mxyoedema
Medical normalisation of hormonal status
- Replacement with Levo-thyroxine T4 (Eltroxin 50 & 100microg tab) 6-7 day half life.
- Elective 25-50microg/day increases fortnightly until clinical and biochemically
euthyroid.
- Emergency 500microg to saturate Thyroid Binding Globulin then 100microg/day
- Never replace with T3 - supra physiological and associated with death (Toft NEJM)
Assessment and treatment of end organ disease
Cardiovascular
Depression of the myocardial function is due to protein and mucopolysaccharide
deposition within the myocardium and depression of intracellular myocardial metobolism.
The cardiac output is decrease because of a bradycardia and a decreased stroke volume,
decreased blood volume and baroreceptor dysfunction. Pericardial effusions may accompany
the hypothyroidism.
- ECG - Will show small complexes which do not distinguish between poor myocardial
contraction and pericardial effusion
- ECHO - to assess LV function and the degree of myocardial compromise due to a
pericardial effusion.
Respiratory
There is always some degree of hypoventilation with the ventilatory response to hypoxia
and hypercarbia being significantly impaired. These patients are increadibly sensitive to
all sedative drugs with the possibility of precipitating respiratory failure.
- Chest X Ray for evidence of aspiration
- Arterial blood gas for baseline oxygenation and ventilation
Hepatic and Renal function
- Renal clearance of drugs is unpredictably altered
- Urea and electrolytes to assess hyponatraemia due to the disease and associated
mineralocorticoid deficiecy, hypokalaemia, hypomagnisaemia and hypophosphataemia are
relatively common.
- Hepatic clearance of drugs is impaired
Thermoregulation
These patients are very prone to hypothermia because of lowered metabolic rate and
lowered heat production.
Intra-operative management
All necessary drugs available especially for thyroid storm (Lugol's, PTU, cortisol,
Esmolol, Digoxin, Verapamil, Lasix) or myxoedema coma.
Check all machines and anaesthetic equipment
Monitoring
- Temperature for hypo or hyperthermia
- ECG for arryhthmias and ischaemia
- Non Invasive Blood pressure
- Peripheral oxygen saturation
- End tidal carbon dioxide
- Muscle relaxation
- Blood glucose
- Central venous pressure and arterial line are indicated in patients with decreased
cardiac reserve
Anaesthetic aims
- Prevent the majority of the sympathetic response to surgery
- Avoid drugs that stimulate the sympathetic nervous system
- Regional anaesthesia can be used to good effect but solutions must not contain
adrenaline.
Positioning
- Limited access to the patient mandates careful attention to good intravenous access
- Excellent eye protection especially with proptosis and exopthalmos
- Careful padding around an inflatable shoulder support. This allows the support to be
deflated at the end of the surgery, allowing good surgical closure.
- 30 o head up tilt int he neutral position with elevation of the legs minimise
venous congestion and surgical bleeding. This can be associated with venous air embolism
Airway management
- There is usually a good laryngeal visualisation however if suspected then fiberoptic
laryngoscopy should be considered
- A wide range of endotracheal tubes must be available because fo the potential for
tracheal narrowing.
- Modern endotracheal tubes provide ample resistance to surgical compression. There is no
longer any need to use a re-inforced endotracheal tube. The old red rubber tubes were very
prone to being compressed by surgical manipulation.
- Visualisation of cord movement at end of surgery. This must be appropriate ie moving
apart when chest rises indicating inspiration (paralysed cords will close on inspiration)
Post operative management
- 24 hours of intensive nursing observation for early detection and treatment of
complications
- Hourly charting of temperature, heart rate, ECG, blood pressure and mental state.
- Four hourly documentation of electrolytes and calcium levels, looking for the following
complications
- Recurrent Laryngeal Nerve paralysis or tracheomalacia may result in airway obstruction
needing emergency re-intubation or tracheostomy
- Haematoma formation may result in associated laryngeal oedema and or spasm causing
respiratory distress
- Removal of staples and sutures
- Careful assessment of bleeding profile
- Surgical consultation for re-exploration of surgical site.
- Hypocalcaemia following parathyroid removal may be transient and asymptomatic or may
present as stridor due to laryngospasm.
- Symptoms - Tetany, Trousseau's & Chvostek's signs, hypotension, cardiac failure,
prolonged Q-T interval
- Treatment - CaCl 2.5 - 5 mg/Kg = 0.2 - 0.5 ml/Kg of 10% solution followed by a
continuous drip with close monitoring of ionised Ca2+ levels
- Mg2+ should also be replaced 1mmol/Kg in 24 hrs. 1g MgSO4 = 8.1 meq = 4mmol
- If the patient is tetanic give 2-3g in 50ml 5% dextrose over 5 minutes then 4-6g over
the next 2-3 hrs.
- Lymphatic duct damage,
- Damage to the cervical sympathetic trunk, phrenic nerve or spinal accessory nerve.
- Thyroid storm
- Continue pre surgery medication
- Thionamide antithyroid drugs are continued for 6-7 days post surgery
- Adrenergic blockade is continued for 7-10 days post surgery
- T4 is re-instituted when the patient can take orally
- Continue analgesia and anti-emesis medication.
- Morphine patient controlled analgesia
- Pethidine 1-2 mg/kg intramuscularly every 4 hours
- Cyclizine (Valoid) 50mg intramusculary 6 hourly
- Continue O2 supplementation as 40% via a venturi mask for 2 hrs
- Position the patient in a comfortable bed with the head elevated 20 o and in a
neutral position.
Thyroid Storm
Definition
Thyroid storm is a life threatening, abrupt exacerbation of hyperthyroidism caused by the
sudden excessive release of thyroid gland hormones into the circulation. It can be
precipitated by surgical stress, but is more common 6-18 hours post operatively. The
highest risk is in patients undergoing emergency surgery.
Diagnosis
- High degree of clinical suspicion.
- No diagnostic laboratory tests
- Rapid elevation in core temperature >41oC - generally regarded as essential to the
diagnosis
- Abrupt onset of sinus tachycardia (often >160 beats per minutes)
- Arrhythmias - atrial fibrillation, premature ventricular contractions and ventricular
fibrillation
- Sudden onset of cardiac failure with profound hypotension and pulmonary oedema
- Mental changes ranging from agitation to psychosis and coma
- Patient appearance (enlarge thyroid; exopthalmos)
- Electrolyte abnormalities
- Hypercalcaemia
- Hypokalaemia
- Differentiate from malignant hyperthermia
- Metabolic acidosis less severe
- Rhabdomyolosis less severe
- Hypoxaemia less severe
- Other differential diagnoses
- Sepsis
- Phaeochromocytoma
- Acute drug intoxication - cocaine and amphetamines
- Central anticholinergic syndrome
- Delirium tremens
- Neuroleptic malignant syndrome
Treatment
As with all flow diagrams the following is presented step by step. Help should be sent
for immediately and as many steps as possible should be performed simultaneously
- Provision of supportive measures
- Ensure oxygenation and ventilation
- Establish invasive cardiovascular monitoring - Central Venous Pressure, arterial line
- Optimise haemodynamics
- Furosemide and morphine for the treatment of pulmonary oedema
- Monitored fluid supplementation against the central venous pressure
- Inotropic support under ECG monitoring
- Collect blood for thyroid hormone and TSH assays prior to treatment
- Identification and treatment of precipitating cause, usually infections
- Actively cool the patient
- Avoid Acetylsalicylate (displaces T4 from TBG)
- Iced saline infusion and lavage body cavities with iced saline (PNGT and rectal catheter
irrigation)
- Place ice over the neck, in the axilla and in the groin. To avoid causing an ice burn it
is best to use an ice slurry.
- Additional support
- Maintain high caloric intake with dextrose containing fluids
- Monitor and treat electrolyte abnormalities
- Vitamin supplementation - especially thiamine infusions (100mg per 24 hour period)
- Prevention of thyroid hormone effects
- Start intravenous infusion of a beta blocker.
- Propanolol (0.05-0.1mg/Kg/6hourly) Start with small doses (0.5mg) to avoid precipitating
cardiac failure, Maintain the heart rate at an acceptable level Antagonises the effect of
thyroid hormones and the hypersensitivity to the action of the catecholamines. Inhibits
the peripheral conversion of T4 to T3
- Esmolol (5-300 microg/Kg/min) Does not prevent the conversion of T4 to T3 Advantageous
in reactive airways disease and cardiac failure
- Reserpine 2.5-5.0mg IMI 4-6 hourly should be reserved for propanolol resistant storm
- Intravenous steroids
- Cortisol 100-200mg 8 hourly
- Dexamethasone 5mg 12 hourly Inhibits the conversion of T4 to T3
Correction concommitant glucocorticoid deficiency
- Specific antithyroid drugs
- Propylthiouracil 1g PNGT followed by 200mg 6 hourly PNGT Inhibits the conversion of T4
to T3 (Effect apparent within 24 hours) Prevents the release of further thyroid hormones
(Effect apparent within 24 hours) Prevents the iodination and oxidative coupling,
preventing the formation of further thyroid hormones (Requires several days for effect)
- Methimazole 100mg PNGT followed by 20mg 12 hourly PNGT Not well absorbed It does not
inhibit peripheral conversion of T4
- Iodide - 30mg (5drops) of lugol's iodine one hour after propylthiouracil. Repeated eight
hourly until the patient is stable Prevents the release of T4 by TSH (Effect apparent
within 24 hours) Transiently inhibits iodine organification and prevents the formation of
further thyroid hormones (Wolff-Chaikoff effect)
- Lithium 500-1500mg daily Blocks thyroid hormone release Plasma exchange Reserved for
refractory cases, following 24-48hours of aggressive conventional therapy.
- Dantrolene 2.5mg/kg starting dose Symptomatic improvement when used to treat
"MHS"
Mxyoedemic Coma
Definition
A rare complication of hypothyroidism manifesting as profound lethargy or coma,
spontaneous hypothermia (less than 35oC), hypoventilation and congestive cardiac failure
Diagnosis
- Features of chronic hypothyroidism are usually present Puffy face, large tongue, coarse
dry skin, carotenaemia, coarse sparse hair
- Additional features often present Seizures, stupor, coma
- Hypoventilation with airway obstruction
- Psychotic behaviour
- Hypothermia
- Hypotension
- Bradycardia
- Markedly delayed tendon reflexes
- Laboratory findings
- Hyponatraemia
- Hypoglycaemia
- Acidosis
- Elevated TSH with low T4
Treatment
- Ensure oxygenation and ventilation
- Establish invasive cardiovascular monitoring - CVP, art line
- Thyroxine (T4 = Eltroxin) 500 microg PNGT followed by 100 microg PNGT per day
- Large doses are needed initially to saturate the thyroid binding globulin
- Tri-iodothyrodine (T3 = Tertroxin) IVI creates supraphysiological levels associated with
arrythmias and ischaemia
- Peripheral conversion of T4 to T3 is unrelated to thyroid status and is regulated
differently in different tissues.
- Careful maintenance of blood pressure
- Careful fluid replacement is mainstay of treatment
- Poor response to inotropic agents
- Combination of inotropes and thyroid hormones can cause severe arrhythmias
- Correct hyponatraemia
- Free water restriction
- If Na+ <115mmol/l use Normal saline or Hypertonic saline 200mls 5% NaCl over 6 hours
- Hydrocortisone 300mg/day IVI
- Stabilise glucose with a glucose infusion associated with 100mg Thiamine a day
- Non aggressive rewarming over 2-4 days
- Prevention of further heat loss
- Warmed fluids
- No External warming devices
- Careful titration of sedation
- Increased sensitivity to narcotics, anaesthetics and tranquillisers
- Identification and treatment of precipitating factor, usually infection

